Abstract
Objective
An important information source for pharmacotherapy in populations at risk is drug labelling. We compared the recommendations for patients with renal insufficiency included in German drug labellings with evidence from the literature.
Methods
From the 120 drugs with the highest turnover in a large university hospital, all drugs with pharmacokinetics independent of renal function (n=48) and those with substantial accumulation in renal failure (n=28) were identified. For both groups of compounds, pharmacokinetic and pharmacodynamic aspects relevant for dose individualisation in those with renal insufficiency were extracted from the literature and compared with the information given in the German drug labelling.
Results
Over half of the labellings (15 of 26) of non-accumulating drugs without renal adverse drug reactions contained no dose recommendation for patients with renal insufficiency. The labelling of nephrotoxic compounds that do not accumulate included more frequently a recommendation to adapt the dose or to monitor than the labelling of drugs without nephrotoxic potential (15 of 22 versus 5 of 26, P=0.002). For over half of accumulating drugs (16 of 28), the dose given in the labelling depends primarily on creatinine clearance. The ratio between the labelling dose and the dose based on the pharmacokinetic concept to achieve identical plasma concentrations (Q 0 concept) differed widely (0.4–2).
Conclusions
When renal failure had no impact on dosing, information was often missing. Such information is however important to differentiate, whether no dose adaptation is necessary or no information is available. If dose adjustment is required, application of a uniform concept is desirable.
Similar content being viewed by others
Introduction
Adverse drug reactions are a very frequent [12] and often preventable [1] event challenging the effectiveness of drug therapy. For drugs eliminated primarily unchanged by the kidney, the risk of dose-dependent adverse drug reactions increases with decreasing renal function [10] and can be reduced by dose adjustment [17]. On average each hospitalised patient is prescribed one drug eliminated predominantly by the kidney and every sixth has an estimated creatinine clearance ≤50 ml/min [9]. Thus, inappropriately high doses in those with renal insufficiency may be a frequent cause of adverse drug reactions.
An important information source for the management of pharmacotherapy in such populations at risk is the drug labelling, i.e. the document written by the marketing authorisation holder and approved by the regulatory authority [3, 15]. Depending on the country of origin, this document is also called Summary of Product Characteristics, Data Sheet or Prescribing Information. The drug labelling may be outdated, as shown for information on initial doses of antihypertensives [18] or management of overdose [15]. In a recent evaluation, the overwhelming majority of drug labellings (70%) did not contain dose recommendations for patients with renal failure [20]. In daily practice, not only are dose recommendations for drugs mainly cleared by the kidneys important but also corresponding statements for drugs whose doses do not need to be reduced and to which no special precautions apply. The study by Spyker and colleagues [20] did not assess information quality nor did, to the best of our knowledge, any other study assess dose recommendations given in drug labelling for patients with renal failure. In the current study, we compared the recommendations for patients with renal insufficiency included in German drug labellings with the evidence from the literature.
We based our comparison on a pharmacokinetic concept, the Q 0 concept [4], and the propensity of the drug to elicit renal adverse drug reactions. Q 0 is the fraction of the bioavailable dose that is eliminated extrarenally. With the drug-specific Q 0 value and creatinine clearance, individual elimination capacity can be estimated and dose and/or dosing interval can be adjusted [4]. We focused our comparison on (1) drugs that accumulate modestly to markedly in those with renal insufficiency (Q 0≤0.5) and therefore have an increased risk to cause dose-dependent adverse drug reactions [10] without dose reduction and (2) drugs that do not accumulate in those with renal insufficiency (Q 0 of parent compound and—if present—active metabolites ≥0.7) and whose dosage does not need adjustment.
Methods
Inclusion of drugs
A list of all drug preparations and their turnover in terms of dispensed units during 2002 in the University Hospital Heidelberg was obtained from the hospital’s pharmacy. We intended to include labellings of drugs with the highest number of dispensed units rather than to use a randomization approach. Starting with the active ingredients with the highest turnover, the first 120 were included to which no exclusion criterion applied (blood substitute n=1; electrolyte n=13; herbal drug n=1; immunoglobulin n=0; local effect n=15; nutritional drug n=1; compound usually administered as a single dose n=3; vaccine n=0; vitamin n=4). The top 120 included drugs comprised around 50% of all dispensed units during 2002, the 38 excluded around 30%. Around two-thirds of the excluded dispensed units belonged to the category of electrolytes.
Evaluation of evidence
Relevant information was extracted from both Drugdex [11], which contains regularly updated evidence-based drug monographs, and the German drug labelling [8]. If several labellings were available, a non-generic product with oral administration was chosen. The extracted information consisted of pharmacokinetic and pharmacodynamic aspects, which are relevant for dose individualisation in patients with renal insufficiency, i.e. Q 0 of the parent drug or its active metabolite in case of a prodrug, formation of active metabolite(s) and their Q 0, and renal adverse drug reactions (i.e. reactions affecting the structure and/or the function of the kidney, which might therefore worsen a pre-existing kidney disease). Inter-rater agreement for data acquisition (n=30 consisting of 15 Drugdex monographs and 15 labellings) had a κ coefficient of 0.86 and 0.93 for presence/absence of active metabolites and renal adverse drug reactions, respectively, and was 97% for the estimated Q 0 value category. Data acquisition was performed by persons with a degree in either medicine, pharmacy or biology.
Q 0 was estimated from both the pharmacokinetic parameters in volunteers with normal renal function reported in Drugdex [11] and from the values reported in the labelling [8]:
In addition, the Q 0 value was available for 92 of 120 drugs in one or two standard lists [5, 21].
For each aspect, the information of the different sources was compared and combined by one author (a physician or a pharmacist), and this evaluation reviewed by another author. Discrepancies were resolved by discussion. To maximise consistency, the second review was performed by only two persons (J.R., M.M.F.), both with several years of experience in the field of clinical pharmacology. In case of contradictory or missing information, additional sources (including original publications) were consulted. If the estimated Q 0 was ≤0.5, studies describing the pharmacokinetics in patients with different degrees of renal impairment were searched, linear regression of total clearance or half-life versus creatinine clearance was performed and Q 0 calculated [4]. Finally, 120 labellings [8], 119 Drugdex monographs [11], 30 other drug monographs [6, 14] and 76 original publications were consulted next to the two lists of Q 0 values [5, 21]. The most recent date of revision/preparation of the labellings was between July 1994 and April 2004. This date was 2001 or later for 100/120 labellings. The most recent date of revision/preparation of the Drugdex monographs was between March 1998 and September 2003. This date was 2001 or later for 114 of 119 monographs. Drug-specific listings of the references are available under http://www.dosing.de. This evaluation of the evidence was the gold standard to which the drug labelling was compared.
Comparison with drug labelling
Included in the comparison were all 76 drugs that do not accumulate in those with renal insufficiency (Q 0 of parent compound and—if present—active metabolites ≥0.7, n=48) and those that accumulate modestly (0.3>Q 0≤0.5, n=9) or markedly (Q 0≤0.3, n=19). Excluded were 44 drugs whose Q 0 is unknown (n=8), drugs to which the Q 0 concept is not applicable (thiazides, loop diuretics and metoclopramide, n=4), drugs with possible accumulation of active metabolite (Q 0≥0.7 and active metabolite whose Q 0 is unknown or <0.7, n=28) and drugs with 0.5>Q 0<0.7 (n=4).
The drug labelling of the 76 included compounds was analysed independently by two reviewers for dose specifications, any other management recommendations, and absolute contraindications (i.e. the drug must never be given under the specified circumstances) in patients with renal insufficiency. The labelling sections dosage, contraindications, precautions and pharmacokinetics were evaluated. Recommendations for dialysed patients were not considered.
For drugs, that accumulate in those with renal insufficiency and whose dose is given as a function of creatinine clearance in the drug labelling, the dose in the labelling was compared with the dose based on the Q 0 concept [4]:
Because with a solid preparation this calculated dose cannot be administered exactly, it was rounded to the next higher practicable dose. Dose adjustment was always calculated for the lowest dose of the dose range recommended in the labelling for normal renal function. These calculations considered the available strengths (including intravenous and oral preparations) and a usual dosing interval (i.e. every 8, 12 or 24 h). In case of combination preparations, only the active ingredient with the higher Q 0 value was included in the comparison. This ingredient entails a smaller dose reduction than the active ingredient with the lower Q 0 value. Thus, all the rules that were considered when calculating the dose based on the Q 0 concept were governed by the aim to avoid underdosage. Finally, the ratio between the labelling dose and the dose based on the Q 0 concept was calculated for different degrees of renal impairment.
Results
Of 48 labellings of drugs that were classified as not accumulating in renal failure, 11 (23%) included an explicit statement that the dose needs not be adjusted. In 35%, no information with respect to dosing in renal failure was given (Table 1). The labelling of compounds that may elicit renal adverse drug reactions included more frequently an absolute contraindication and/or a recommendation to monitor drug effects or adjust the dose than drugs without known propensity to elicit renal adverse drug reactions (15 of 22 versus 5 of 26, P=0.002 for χ 2-test with Yates’ correction).
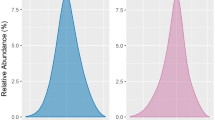
The labelling of all 28 drugs that accumulate in patients with renal insufficiency included a recommendation on how to proceed in patients with renal failure. Of these, 1 drug (metformin) is contraindicated, the dosage of 7 depends primarily on clinical endpoints or lab parameters (bisoprolol, clonidine, angiotensin-converting enzyme inhibitors, allopurinol, lithium), for 2 drugs only the maximal dosage is given, for another 2 drugs dosage is indicated as a function of serum creatinine, and for 16 drugs dosage depends primarily on creatinine clearance. For 9 of these 16 drugs, the ratio between the labelling dose and the dose based on the Q 0 concept could be calculated (Fig. 1). For 4 of the 9 drugs, this ratio is between 0.67 and 1.5 (i.e. multiplication or division by ≤1.5). For varying clearance ranges of the other 5 drugs, the ratio even lies between >1.5 or 2 or 0.5 and <0.67 (i.e. either multiplication by a factor of >1.5–2 or division by a factor of >1.5–2). Seven drugs were not included in this comparison: for three not enough data is published to calculate Q 0 from linear regression (aciclovir, alizapride, amisulpride), one was excluded, because the labelling dose in patients with renal insufficiency depends on duration of therapy (trimethoprim) and one, because the dose in those with renal insufficiency is given as a range (venlafaxine). Finally, in case of the combination products imipenem/cilastatin and piperacillin/tazobactam only the drugs with the higher Q 0 value, i.e. imipenem and piperacillin were included, which are in addition mainly responsible for the therapeutic effect. Hence, cilastatin and tazobactam were also excluded.
Discussion
The drug labelling, i.e. the monograph written by the marketing authorisation holder and approved by the regulatory authority, should provide a summary of the essential scientific information needed for the safe and effective use of a drug product [7, 13]. The aim of this study was to compare the recommendations given in the German drug labelling for the large population of patients with renal insufficiency with the available evidence. We focused our comparison on the subset of frequently used drugs which were either substantially accumulating in those with renal insufficiency or not at all.
For drugs that do not accumulate in patients with renal insufficiency, one in four labellings correctly states that no dose adaptation is necessary, whereas such information is completely lacking for one-third of these compounds. In the subgroup of compounds without nephrotoxic potential, over half of the labellings contain no recommendation at all on how to proceed and may thus not satisfy the information needs of treating physicians in daily practice. The propensity of a drug to elicit renal adverse drug reactions appears to prompt precautionary recommendations, because 68% of the labellings of such drugs include recommendations such as dose adaptation, monitoring or a contraindication. For compounds without nephrotoxic potential that are not accumulating in renal failure, this proportion decreases to 20%. A useful way to characterise drugs that may elicit renal adverse drug reactions is to mention that renal disease has no influence on plasma concentration and to state which parameter has to be monitored or is influenced by renal disease. For only two drugs, such information was given. The labelling of atorvastatin recommends monitoring creatine kinase [19]. The labelling of rofecoxib states that renal perfusion may be decreased due to inhibition of prostaglandin synthesis [22].
While the labelling of all drugs with significant renal elimination of its active compound includes a management recommendation for patients with renal insufficiency, the manner how to proceed differs widely. For one-quarter of the drugs that accumulate in patients with renal insufficiency, the labelling dose depends primarily on clinical endpoints or lab parameters. For two drugs, the dose is given as a function of serum creatinine, which should not be used as a sole indicator of renal function [16] because it may underestimate the degree of renal impairment particularly in elderly normal weight patients. For over half of the drugs that accumulate in patients with renal insufficiency, the dose given in the labelling depends primarily on creatinine clearance. The ratio between the labelling dose and the dose based on the Q 0 concept differs widely between 0.4 and 2. For drugs with a narrow therapeutic window (vancomycin, gabapentin) or with well-known serious dose-dependent adverse drug reactions (imipenem) [17], the labelling dose was identical to or lower than the dose calculated with the Q 0 algorithm. However, for well tolerated beta-lactam antibacterials, the labelling recommends a dose that was never smaller than and frequently considerably higher than the dose based on the Q 0 concept, often reaching values required to maintain plasma concentrations in the range of patients with normal renal function. This might be guided by the concept of avoiding underdosage of the well-tolerated antibacterials. Thus, the dose recommendation in the labelling is obviously not only based on pharmacokinetic considerations. Indeed, it appears likely that drug-specific aspects influence the recommendation. Examples are avoidance of underdosage in case of well-tolerated drugs where immediate efficacy is of prime importance and minimisation of risk of adverse drug reactions for less-well-tolerated drugs. However, because it is not evident to the treating physician which aspects have been taken into account in the dose appearing in the labelling, the application of a uniform concept may be preferable, yielding recommendations for different drugs comparable. Moreover, it might also help to reduce avoidable costs.
Evidence-based guidelines are developed and regularly updated for treatment of specific diseases. To the best of our knowledge no such “guidelines” covering dose individualisation in populations at risk are available. This situation coupled with the fact that drug labelling is a pertinent knowledge source for treating physicians [2, 3, 15] emphasises the importance of drug labelling. To be a reliable source, the evidence must be evaluated according to the same principles for all drugs, and similar constellations must entail similar recommendations. Whenever the Q 0 concept is applicable (e.g. absence of a deep second compartment, patients without continuous or intermittent renal replacement therapy), we suggest that the recommended maintenance doses are based on the calculated Q 0 value. This dose leads, on average, to the same drug concentration as in patients without renal insufficiency and is thus a first and useful “informed guess” even for those drugs for which concentration is monitored or dosage is mainly based on clinical endpoints. Treating physicians may increase or decrease this dose depending on patient-specific factors such as the severity of the disease. To satisfy information needs, the labelling should not only include recommendations when the dose has to be adapted or any other precautions apply, but clearly state when no special precautions in patients with renal insufficiency are necessary.
References
Bates DW, Cullen DJ, Laird N, Petersen LA, Small SD, Servi D, Laffel G, Sweitzer BJ, Shea BF, Hallisey R, Vander Vliet M, Nemeskal R, Leape LL (1995) Incidence of adverse drug events and potential adverse drug events. JAMA 274:29–34
Bergk V, Gasse C, Schnell R, Haefeli WE (2004) Requirements for a successful implementation of drug interaction information systems in general practice: results of a questionnaire survey in Germany. Eur J Clin Pharmacol 60:595–602
Connelly DP, Rich EC, Curley SP, Kelly JT (1990) Knowledge resource preferences of family physicians. J Fam Pract 30:353–359
Dettli L (1984) The kidney in pre-clinical and clinical pharmacokinetics. Jpn J Clin Pharmacol Ther 15:241–254
Dettli L (1996) Pharmakokinetische Daten für die Dosisanpassung. In: Grundlagen der Arzneimitteltherapie. Herausgegeben durch die Sektion Klinische Pharmakologie der Schweizerischen Gesellschaft für Pharmakologie und Toxikologie. 14. Auflage. Basel: Documed, pp 13–21
Dollery C (ed) (1999) Therapeutic drugs, 2nd edn. Churchill Livingstone, Edinburgh
European Commission (1999) A guideline on the summary of product characteristics. Final—revision 0. Available at: http://pharmacos.eudra.org/F2/eudralex/vol-2/C/SPCGuidRev0-Dec99.pdf. Accessed December 7, 2004
FachInfo-Service, Fachinformationsverzeichnis Deutschland. BPI Service GmbH. http://www.fachinfo.de/. Accessed between 27 Feb 2003 and 30 Jan 2004
Falconnier AD, Haefeli WE, Schoenenberger RA, Surber C, Martin-Facklam M (2001) Drug dosage in patients with renal failure optimized by immediate concurrent feedback. J Gen Intern Med 16:369–375
Jick H (1977) Adverse drug effects in relation to renal function. Am J Med 62:514–517
Klasco RK (ed) DRUGDEX System. MICROMEDEX Inc. Greenwood Village, Colorado, versions used: first quarter 2003 – first quarter 2004
Lazarou J, Pomeranz BH, Corey PN (1998) Incidence of adverse drug reactions in hospitalized patients. A meta-analysis of prospective studies. JAMA 279:1200–1205
Marroum PJ, Gobburu J (2002) The product label: how pharmacokinetics and pharmacodynamics reach the prescriber. Clin Pharmacokinet 41:161–169
Medscape DrugInfo. http://www.medscape.com/druginfo. Accessed on 5 September 2003 and 21 April 2004
Mullen WH, Anderson IB, Kim SY, Blanc PD, Olson KR (1997) Incorrect overdose management advice in the Physicians’ Desk Reference. Ann Emerg Med 29:255–61
National Kidney Foundation (NKF) Kidney Disease Outcome Quality Initiative (K/DOQI) Advisory Board (2002) K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Kidney disease outcome quality initiative. Part 5. Evaluation of laboratory measurements for clinical assessment of kidney disease. Am J Kidney Dis 39:S76–S110
Pestotnik SL, Classen DC, Evans RS, Stevens LE, Burke JP (1993) Prospective surveillance of imipenem/cilastatin use and associated seizures using a hospital information system. Ann Pharmacother 27:497–501
Rajpal A, Reidenberg MM (2003) Drug labeling should be kept current. Clin Pharmacol Ther 73:4–6
Sortis, Prescribing Information of January 2003. In: FachInfo-Service, Fachinformationsverzeichnis Deutschland. BPI Service GmbH. http://www.fachinfo.de/. Accessed on 3 Nov 2003
Spyker DA, Harvey ED, Harvey BE, Harvey AM, Rumack BH, Peck CC, Atkinson AJ Jr, Woosley RL, Abernethy DR, Cantilena LR (2000) Assessment and reporting of clinical pharmacology information in drug labeling. Clin Pharmacol Ther 67:196–200
Taeschner W, Vozeh S (1997) Pharmacokinetic drug data. In: Speight TM, Holford NHG (eds) Averyás drug treatment, 4th ed. adis International Appendix A, pp 1629–1664
Vioxx, Prescribing Information of August 2003. In: FachInfo-Service, Fachinformationsverzeichnis Deutschland. BPI Service GmbH. http://www.fachinfo.de/. Accessed 13 Nov 2003
Acknowledgements
We are grateful to Peter Martin for excellent programming of the Access database which was used for evaluation of evidence. V.B. was supported by the Graduiertenkolleg 793 (German Research Foundation, DFG).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Martin-Facklam, M., Rengelshausen, J., Tayrouz, Y. et al. Dose individualisation in patients with renal insufficiency: does drug labelling support optimal management?. Eur J Clin Pharmacol 60, 807–811 (2005). https://doi.org/10.1007/s00228-004-0852-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-004-0852-y