Abstract
Background
Seniors frequently struggle during the transition home following an acute hospitalization resulting in frequent rehospitalizations. Studies consistently show a lack of comprehension of discharge instructions.
Objectives
To determine the frequency of low cognition at hospital discharge among community dwelling seniors and the changes in cognition that occur one month following hospitalization.
Design
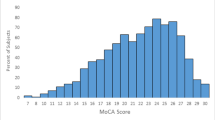
Face-to-face surveys were performed at hospital discharge and one month later in the home of the subject. The Mini-Mental Status Examination (MMSE), Backward Digit Span, and 15 Word Immediate and Delayed Recall Tests were used to evaluate cognition. Low cognition was determined to be a score of less than 25 on the MMSE for subjects with high school education and less than 18 for subjects with less than high school education.
Participants
Two hundred community-dwelling seniors ≥ 70 years, admitted to acute medicine services >24 hours, consenting to their own procedures, not having previously documented cognitive loss, and not admitted for cognitive changes.
Results
Upon hospital discharge, 31.5% of subjects had previously unrecognized low cognition. One month later, 58% of these patients no longer had low cognition (p < 0.001). Of those subjects with low cognition, the MMSE improved by an average of 4 points one month post-discharge. Within the MMSE, subjects experienced significant improvements in the areas of orientation, registration, repetition, comprehension, naming, reading, writing, and calculation.
Conclusion
Low cognition at discharge is common among elderly patients without dementia, and cognition often improves one month post-hospitalization. Seniors may not comprehend discharge instructions, and patient self-management may be better taught as an outpatient following discharge rather than at the time of hospital discharge. Discharge interventions should incorporate screening of seniors for low cognition prior to hospital discharge to provide optimal transitional care.

Similar content being viewed by others
References
Bodenheimer T, Bodenheimer T. Coordinating care–a perilous journey through the health care system. N Engl J Med. 2008;358(10):1064–1071.
Coleman EA. Falling through the cracks: Challenges and Opportunities for Improving Transitional Care for Persons with Continuous Complex Care Needs. J Am Geriatr Soc. 2003;51:549–555.
Chugh A, Williams MV, Grigsby J, et al. Better transitions: improving comprehension of discharge instructions. Front Health Serv Manage. 2009;25(3):11–32.
Jencks SF, Williams MV, Coleman EA, Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med. 2009;360(14):1418–1428.
Marcantonio ER, McKean S, Goldfinger M, Kleefield S, Yurkofsky M, Brennan TA. Factors associated with unplanned hospital readmission among patients 65 years of age and older in a Medicare managed care plan. Am J Med. 1999;107(1):13–17.
Gillick MR, Serrell NA, Gillick LS. Adverse consequences of hospitalization in the elderly. Soc Sci Med. 1982;16:1033–1038.
Naylor MD. Transitional care of older adults. Annu Rev Nurs Res. 2003;20:127–147.
Coleman EA, Smith JD, Raha D, Min SJ. Posthospital Medication Discrepancies. Arch Intern Med. 2005;165:1842–1847.
Creditor MC. Hazards of hospitalization of the elderly. Ann Intern Med. 1993;118:219–223.
Gray SL, Mahoney JE, Blough DK. Adverse drug events in elderly patients receiving home health services following hospital discharge. Ann Pharmacother. 1999;33:1147–1153.
Chawla S, Pastores SM, Hassan K, et al. ICU admissions after actual or planned hospital discharge: incidence, clinical characteristics, and outcomes in patients with cancer. Chest. 2009;136(5):1257–1262.
Clemens EL. Multiple perceptions of discharge planning in one urban hospital. Health Soc Work. 1995;20(4):254–261.
Williams MV, Coleman E, Williams MV, Coleman E. BOOSTing the hospital discharge. J Hosp Med (Online). 2009;4(4):209–210.
Coleman EA, Smith JD, Frank JC, Min A, Parry C, Kramer AM. Preparing patients and caregivers to participate in care delivered across settings: The care transitions interventions. J Am Geriatr Soc. 2004;52:1817–1825.
Jack BW, Chetty VK, Anthony D, et al. A reengineered hospital discharge program to decrease rehospitalization: a randomized trial. Ann Intern Med. 2009;150(3):178–187.
Jha AK, Orav EJ, Epstein AM, Jha AK, Orav EJ, Epstein AM. Public reporting of discharge planning and rates of readmissions. N Engl J Med. 2009;361(27):2637–2645.
Calkins DR. Davis, R.B., Reiley, P., et al. Patient-Physician Communication at Hospital Discharge and Patients' Understanding of the Postdischarge Treatment Plan. Arch Intern Med. 1997;157:1026–1030.
Maniaci MJ, Heckman MG, Dawson NL, Maniaci MJ, Heckman MG, Dawson NL. Functional health literacy and understanding of medications at discharge. Mayo Clin Proc. 2008;83(5):554–558.
Beers MH, Dang J, Hasegawa J, Tamai IY. Influence of Hospitalization on Drug Therapy in the Elderly. J Am Geriatr Soc. 1989;37:679–683.
Forster AJ. Murff, H.J., Peterson, J.F., Gandhi, T.K., Bates, D.W. The incidence and severity of adverse events affecting patients after discharge from the hospital. Ann Intern Med. 2003;138:161–167.
Forster AJ, Clark HD, Menard A, et al. Adverse events among medical patients after discharge from hospital. CMAJ Can Med Assoc J. 2004;170(3):345–349.
Graf C, Graf C. Functional decline in hospitalized older adults. Am J Nurs. 2006;106(1):58–67. 67–8.
Hickey A, Clinch D, Groarke EP. Prevalence of cognitive impairment in the hospitalized elderly. Int J Geriatr Psychiatry. 1997;12:27–33.
Fields SD, MacKenzie CR, Charlson ME, Perry SW. Reversibility of cognitive impairment in medical inpatients. Arch Intern Med. 1986(146):1593–1596.
Inouye SK, Zhang Y, Han L, Leo-Summers L, Jones R, Marcantonio E. Recoverable cognitive dysfunction at hospital admission in older persons during acute illness. J Gen Intern Med. 2006;21(12):1276–1281.
Inouye S, van Dyck C, Alessi C, Balkin S, Siegal A, Horwitz R. Clarifying confusion: the confusion assessment method. A new method for detection of delirium. Ann Intern Med. 1990;113(12):941–948.
Folstein MF, Folstein SE, McHugh PR. Mini Mental State: A practical method for grading the cognitive state of patient for the clinician. J Psychiatr Res. 1975;12:196–198.
Tun PA Lachman ME. Brief Test of Adult Cognition by Telephone (BTACT) Technical Report. Accessed on February 14,2011. Available at http://www.brandeis.edu/departments/psych/lachman/pdfs/techreport.pdf.
Tun PA Lachman ME. Guidelines on Administration and Scoring of the Brief Test of Adult Cognition by Telephone (BTACT). Accessed on February 14, 2011. Available on http://www.brandeis.edu/departments/psych/lachman/pdfs/btact-admin-scoring.pdf
Acknowledgements
Dr. Lindquist and this study were funded by a grant from the National Institute of Aging (K23AG028439-04). The contents of this publication are solely the responsibility of the authors and do not necessarily represent the official views of the National Institutes of Health. Preliminary data for this paper were presented as an abstract at the Society of General Internal Medicine 2010 National Meeting.
Conflict of Interest
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lindquist, L.A., Go, L., Fleisher, J. et al. Improvements in Cognition Following Hospital Discharge of Community Dwelling Seniors. J GEN INTERN MED 26, 765–770 (2011). https://doi.org/10.1007/s11606-011-1681-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-011-1681-1