Abstract
Background
In 2011, the Veterans Health Administration (VHA) released the Acute Ischemic Stroke (AIS) Directive, which mandated reorganization of acute stroke care, including self-designation of stroke centers as Primary (P), Limited Hours (LH), or Supporting (S).
Objectives
In partnership with the VHA Offices of Emergency Medicine and Specialty Care Services, the VA Stroke QUERI conducted a formative evaluation in a national sample of three levels of stroke centers in order to understand barriers and facilitators.
Design and Approach
The evaluation consisted of a mixed-methods assessment that included a qualitative assessment of data from semi-structured interviews with key informants and a quantitative assessment of stroke quality-of-care data reporting practices by facility characteristics.
Participants
The final sample included 38 facilities (84 % participation rate): nine P, 24 LH, and five S facilities. In total, we interviewed 107 clinicians and 16 regional Veterans Integrated Service Network (VISN) leaders.
Results
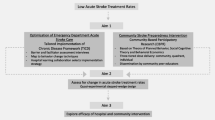
Across all three levels of stroke centers, stroke teams identified the specific need for systematic nurse training to triage and initiate stroke protocols. The most frequently reported barriers centered around quality-of-care data collection. A low number of eligible veterans arriving at the VAMC in a timely manner was another major impediment. The LH and S facilities reported some unique barriers: access to radiology and neurology services; EMS diverting stroke patients to nearby stroke centers, maintaining staff competency, and a lack of stroke clinical champions. Solutions that were applied included developing stroke order sets and templates to provide systematic decision support, implementing a stroke code in the facility for a coordinated response to stroke, and staff resource allocation and training. Data reporting by facility evaluation demonstrated that categorizing site volume did indicate a lower likelihood of reporting among VAMCs with 25–49 acute stroke admissions per year.
Conclusions
The AIS Directive brought focused attention to reorganizing stroke care across a wide range of facility types. Larger VA facilities tended to follow established practices for organizing stroke care, but the unique addition of the LH designation presented some challenges. S facilities tended to report a lack of a coordinated stroke team and champion to drive process changes.
Similar content being viewed by others
References
Veterans Administration HSRD Stroke QUERI Center Annual Report 2012.
Ross JS, Arling G, Ofner S, Roumie CL, Keyhani S, Williams LS, Ordin DL, Bravata DM. Correlation of inpatient and outpatient measures of stroke care quality within veterans health administration hospitals. Stroke. 2011;42(8):2269–2275.
Keyhani S, Arling G, Williams LS, Ross JS, Ordin DL, Myers J, Tyndall G, Vogel B, Bravata DM. The use and misuse of thrombolytic therapy within the Veterans Health Administration. Med Care. 2012;50(1):66–73.
Treatment of Acute Ischemic Stroke (AIS). VHA Directive 2011–038. Department of Veterans Affairs. Veterans Health Administration. November 2, 2011.
Damush TM, Plue L, Bakas T, Schmid A, Williams LS. Barriers and facilitators to exercise among stroke survivors. Rehabil Nurs. 2007;32:253–262.
Sternke E, Burrus N, Daggett V, Plue L, Carlson K, Hershey L, Chumbler N. Improving knowledge and information sharing to promote best practices in stroke care: evaluation of the VA Stroke QUERI Toolkit. Int J Reliab Qual E-Healthc 2013;2(1).
Box T, McDonell, Helfrich C, Jesse R, Fihn S, Rumsfeld J. Strategies from a nationwide health information technology implementation: the VA CART story. JGIM. 2010;25:72–76.
Fonarow G, Zhao X, Smith E, Saver J, Reeves M, Bhatt D, Xian Y, Hernandez A, Peterson E, Schwamm L. Door-to-needle times for tissue plasminogen activator administration and clinical outcomes in acute ischemic stroke before and after a quality improvement initiative. JAMA. 2014;311(16):1632–1640.
Institute of Medicine. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington DC: National Academy Press; 2001.
Ekundayo OJ, Saver, Fonarow GC JL, Schwamm LH, Xian Y, Zhao X, Hernandez AF, Peterson ED, Cheng EM. Patterns of emergency medical services use and its association with timely stroke treatment findings from Get with the Guidelines-Stroke. Cir Cardiovasc Qual Outcomes. 2013;6.
Acknowledgments
This protocol was supported in part by the VA HSRD QUERI Rapid Response Project 11–374, the Genentech Inc. Protocol ML 28238, and the VA Stroke QUERI Center. We appreciate the time and effort of the VA facility clinical providers, staff and administrators, and VISN leaders across the VHA who participated in our interviews.
Role of the Sponsors
The funding organizations had no role in the design or conduct of the study, in the collection, analysis, and interpretation of the data, or in the preparation, review, or approval of the manuscript.
Disclaimer
The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs or the U.S. Government.
Conflict of Interest
We received partial funding for this project from Genentech Inc. The authors declare no other conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 90 kb)
Rights and permissions
About this article
Cite this article
Damush, T.M., Miller, K.K., Plue, L. et al. National Implementation of Acute Stroke Care Centers in the Veterans Health Administration (VHA): Formative Evaluation of the Field Response. J GEN INTERN MED 29 (Suppl 4), 845–852 (2014). https://doi.org/10.1007/s11606-014-3036-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-014-3036-1