Abstract
OBJECTIVE: Previous studies have shown that most medical inpatients receive treatment supported by strong evidence (evidence-based treatment), but they have not assessed whether and how physicians actually use evidence when making their treatment decisions. We investigated whether physicians would change inpatient treatment if presented with the results of a literature search.
DESIGN: Before-after study.
SETTING: Large public teaching hospital.
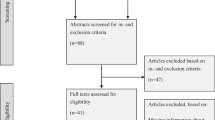
PARTICIPANTS: Random sample of 146 inpatients cared for by 33 internal medicine attending physicians.
INTERVENTIONS: After physicians committed to a specific diagnosis and treatment plan, investigators performed standardized literature searches and provided the search results to the attending physicians.
MEASUREMENTS AND MAIN RESULTS: The primary study outcome was the number of patients whose attending physicians would change treatment due to the literature searches. These changes were evaluated by blinded peer review. A secondary outcome was the proportion of patients who received evidence-based treatment before and after the literature searches. Attending physicians changed treatment for 23 (18%) of 130 eligible patients (95% confidence interval, 12% to 24%) as a result of the literature searches. Overall, 86% of patients (112 of 130) received evidence-based treatments before the searches and 87% (113 of 130) after the searches. Changes were not related to whether patients were receiving evidence-based treatment before the search (P=.6). Panels of peer reviewers judged the quality of patient care as improved or maintained for 18 (78%) of the 23 patients with treatment changes.
CONCLUSIONS: Searching the literature could improve the treatment of many medical inpatients, including those already receiving evidence-based treatment.
Similar content being viewed by others
References
Forsyth G. An inquiry into the drug bill. Med Care. 1963;1:10–16.
Office of Technology Assessment of the Congress of the United States. Assessing the Efficacy and Safety of Medical Technologies. Washington, DC: U.S. Government Printing Office; 1978.
Office of Technology Assessment of the Congress of the United States. The Impact of Randomized Clinical Trials on Health Policy and Medical Practice. Washington, DC: U.S. Government Printing Office; 1983.
Dubinsky M, Ferguson JH. Analysis of the National Institutes of Health Medicare Coverage Assessment. Int J Technol Assess Health Care. 1990;6:480–8.
What Proportion of Healthcare Is Evidence Based? Resource Guide. Available at: http://www.shef.ac.uk/~scharr/ir/percent.html. Accessed July 8, 2003.
Ellis J, Mulligan I, Rowe J, Sackett DL. Inpatient general medicine is evidence based. Lancet. 1995;346:407–10.
Michaud G, McGowan JL, van der Jagt R, Wells G, Tugwell P. Are therapeutic decisions supported by evidence from health care research? Arch Intern Med. 1998;158:1665–8.
Nordin-Johansson A, Asplund K. Randomized controlled trials and consensus as a basis for interventions in internal medicine. J Intern Med. 2000;247:94–104.
Feinstein AR, Horwitz RI. Problems in the “evidence” of “evidence-based medicine.” Am J Med. 1997;103:529–35.
van Weel C, Knottnerus JA. Evidence-based interventions and comprehensive treatment. Lancet. 1999;353:916–8.
Sackett DL, Rosenberg W, Gray JAM, Haynes RB, Richardson WS. Evidence based medicine: what it is and what it isn’t. It’s about integrating individual clinical expertise and the best external evidence. BMJ. 1996;312:71–2.
Smith CA, Ganschow PS, Reilly BM, et al. Teaching residents evidence-based medicine skills: a controlled trial of effectiveness and assessment of durability. J Gen Intern Med. 2000;15:710–5.
Reilly B, Lemon M. Evidence-based morning report: a popular new format in a large teaching hospital. Am J Med. 1997;103:419–26.
Reilly BM, Hart A, Evans AT. Evidence-based medicine: a passing fancy or the future of primary care? Dis Mon. 1998;44:370–99.
Sackett DL, Straus SE, Richardson WS, Rosenberg W, Haynes RB. Evidence-Based Medicine. How to Practice and Teach EBM. 2nd ed. New York, NY: Churchill Livingstone; 2000.
Haynes RB. Of studies, syntheses, synopses, and systems: the “4S” evolution of services for finding the current best evidence. ACP J Club. 2001;134:A11-A13.
Fleiss JL. Statistical Methods for Rates and Proportions. 2nd ed. New York, NY: John Wiley & Sons; 1981:225–33.
Fleiss JL. The Design and Analysis of Clinical Experiments. New York, NY: John Wiley & Sons; 1986:14–5.
Greenhalgh T. “Is my practice evidence-based?” BMJ. 1996;313:957–8.
Guyatt G, Schunemann H, Cook D, Jaeschke R, Pauker S, Bucher H. American College of Chest Physicians. Grades of recommendation for antithrombotic agents. Chest. 2001;119(1 suppl):3S-7S.
Feinstein AR. An additional basic science for clinical medicine: I. The constraining fundamental paradigms. Ann Intern Med. 1983;99:393–7.
Feinstein AR. An additional basic science for clinical medicine: III. The challenges of comparison and measurement. Ann Intern Med. 1983;99:705–12.
Sackett DL. … so little time, and … Evidence-Based Medicine. 1997;2:39.
Del Mar CB, Silagy CA, Glasziou PP, et al. Feasibility of an evidence-based literature search service for general practitioners. MJA. 2001;175:134–7.
Brassey J, Elwyn G, Price C, Kinnersley P. Just in time information for clinicians: a questionnaire evaluation of the ATTRACT project. BMJ. 2001;322:529–30.
Sackett DL, Straus SE. Finding and applying evidence during clinical rounds: the “evidence cart.” JAMA. 1998;280:1336–8.
Guyatt GH, Meade MO, Jaeschke RZ, Cook DJ, Haynes RB. Practitioners of evidence based care. BMJ. 2000;320:954–6.
McColl A, Smith H, White P, Field J. General practitioners’ perceptions of the route to evidence based medicine: a questionnaire survey. BMJ. 1998;316:361–7.
Tomlin Z, Humphrey C, Rogers S. General practitioners’ perceptions of effective health care. BMJ. 1999;318:1532–5.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lucas, B.P., Evans, A.T., Reilly, B.M. et al. The impact of evidence on physicians’ inpatient treatment decisions. J GEN INTERN MED 19, 402–409 (2004). https://doi.org/10.1111/j.1525-1497.2004.30306.x
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2004.30306.x